Ventilators do save lives, but not often. They are a prime example of how expensive end-of-life treatment can be.
Ventilators Are No Panacea For Critically Ill COVID-19 Patients
April 2, 20203:43 PM ET

Jon Hamilton 3-Minute Listen
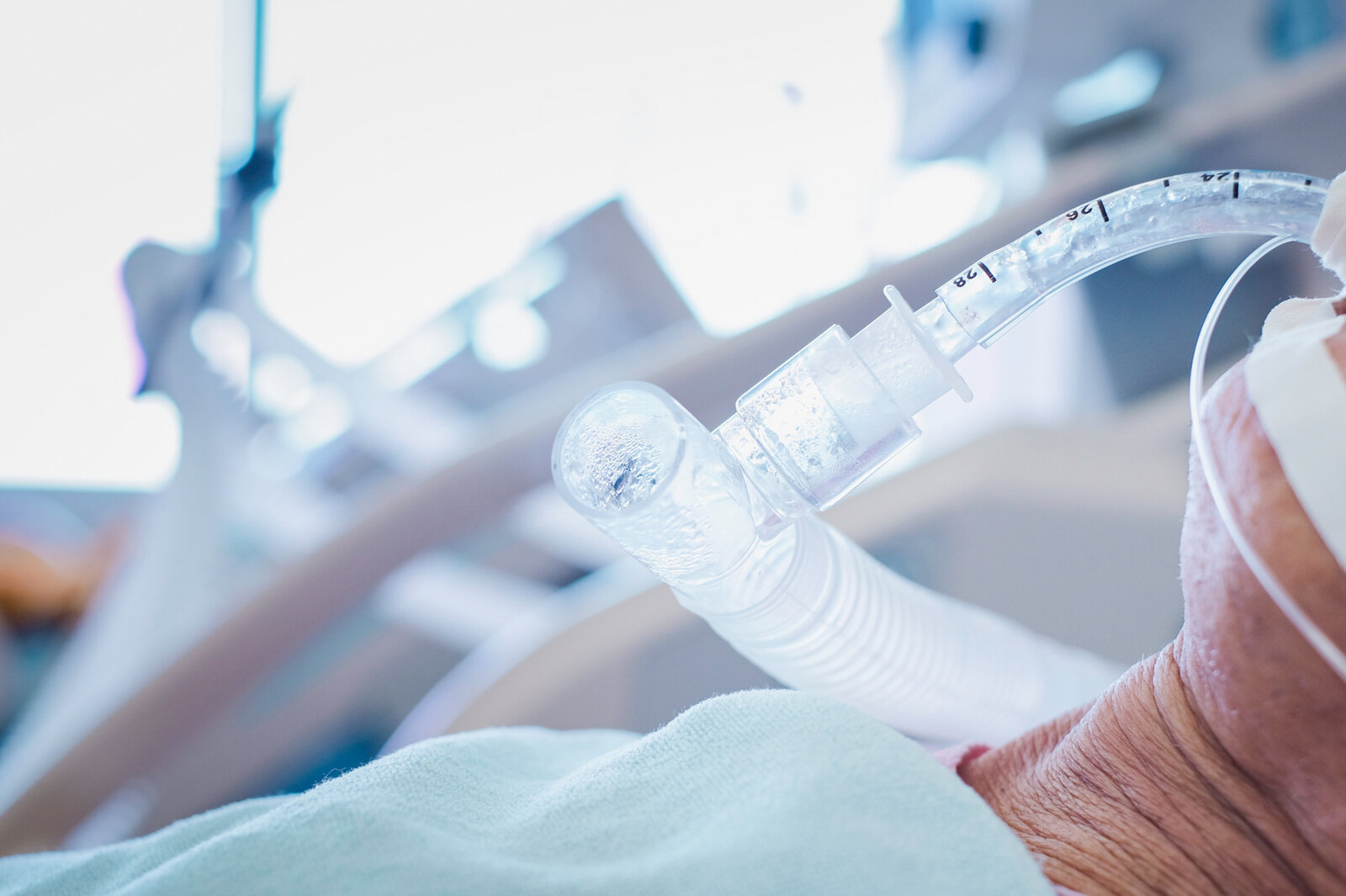
A ventilator can help patients unable to breathe on their own, but the experience of COVID-19 patients has been sobering for doctors. Taechit Taechamanodom/Getty Images
Most coronavirus patients who end up on ventilators go on to die, according to several small studies from the U.S., China and Europe.
And many of the patients who continue to live can’t be taken off the mechanical breathing machines.
“It’s very concerning to see how many patients who require ventilation do not make it out of the hospital,” says Dr. Tiffany Osborn, a critical care specialist at Washington University in St. Louis who has been caring for coronavirus patients at Barnes-Jewish Hospital.
That concern is echoed by Negin Hajizadeh, a pulmonary critical care doctor at the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell on Long Island, N.Y.
“We have had several patients between the hospitals across the Northwell system that have come off the breathing machine,” Hajizadeh says. “But the vast majority are unable to.”
The largest study so far to look at mortality among coronavirus patients on ventilators was done by the Intensive Care National Audit & Research Centre in London. It found that among 98 ventilated patients in the U.K., just 33 were discharged alive.
Sign Up For The New Normal Newsletter
Daily news on the coronavirus crisis and help getting through whatever comes next. We’re in this together.E-mail address
By subscribing, you agree to NPR’s terms of use and privacy policy. NPR may share your name and email address with your NPR station. See Details. This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
The numbers from a study of Wuhan, China, are even grimmer. Only 3 of 22 ventilated patients survived.
And a study of 18 ventilated patients in Washington state found that nine were still alive when the study ended, but only six had recovered enough to breathe on their own.
All the early research suggests that once coronavirus patients are placed on a ventilator, they will probably need to stay on it for weeks. And the longer patients remain on a breathing machine, the more likely they are to die.
“We’re not sure how much help ventilators are going to be,” Osborn says. “They may help keep somebody alive in the short term. We’re not sure if it’s going to help keep someone alive in the long term.”
Patients need a ventilator when their lungs can no longer deliver enough oxygen to keep the body going. And it’s an extreme measure, Osborn says.
“We give sedation so the person goes to sleep. Then we provide a paralytic that stops their breathing,” she says.
Next, a long plastic tube is inserted through the trachea and vocal cords. That allows a machine to deliver small puffs of highly oxygenated air to the lungs.
Unfortunately, Osborn says, “the ventilator itself can do damage to the lung tissue based on how much pressure is required to help oxygen get processed by the lungs.”
And coronavirus patients often need dangerously high levels of both pressure and oxygen because their lungs have so much inflammation.
Another risk from being on a ventilator is that the tube carrying air and extra oxygen to the lungs provides a pathway for dangerous germs. Many ventilated patients get a new lung infection, a problem known as ventilator-associated pneumonia.
Ventilators have been seen as critical to treating coronavirus patients because the devices are very successful when used to treat common forms of pneumonia, says Hajizadeh.

A ventilator alongside medical supplies and a stretcher is displayed before a news conference at the Javits Center in New York City on March 23. John Minchillo/AP
“We treat patients for several days, and then we get the antibiotics into the body and the patient recovers,” she says. “Unfortunately with this COVID-associated pneumonia, there are no treatments that we know work for sure.”
Also, the coronavirus often does a lot more damage to a person’s lungs than pneumonia associated with the flu. “There is fluid and other toxic chemicals, cytokines we call them, raging throughout the lung tissue,” she says.
In some patients, the damage is so bad that even ventilation won’t help. So doctors have sometimes tried an even more extreme measure called extracorporeal membrane oxygenation, or ECMO, which delivers oxygen directly to a patient’s bloodstream.
But this is still a stopgap measure. “Remember, ECMO too is a life-supporting treatment,” Hajizadeh says. “So it’s a bridge while we are allowing the lung to heal itself from a pneumonia.”
But lungs don’t always heal, no matter how much help they get from a machine, Osborn says. So people need to be diligent about social distancing to keep the virus from spreading.
“I know that at times it gets frustrating,” she says. “But it’s really important not only for yourself and your family but for the other people you care about to shelter in place until this is over.”
Osborn should know. When she’s not caring for patients at the hospital, she’s living in a camper to avoid putting her family at risk.